Signed in as:
filler@godaddy.com
Signed in as:
filler@godaddy.com
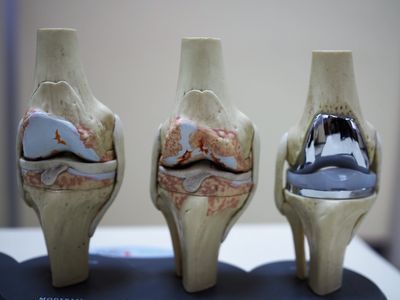
Knee Osteoarthritis (OA) is a very common degenerative knee condition that affects most of us as we age. The cartilage is a smooth gliding surface that allows the knee to move freely, it is made of collagen and cells that hold water tightly. As we age, or sustain cartilage damage, through trauma, infection, rheumatic conditions, this cartilage cannot function fully and begins to deteriorate. This condition may then cause pain, swelling, deformity, stiffness and limited function.
Currently, there is no community available, scientifically proven method of reproducing cartilage or regrowing cartilage in a degenerate knee or reversing the changes of osteoarthritis. The current aims of treatment include prevention, with keeping weight at a healthy BMI, avoiding injuries, especially those associated with ligament injuries like ACL or PCL injuries. Other treatment aims are to slow the progression of the disease through "off-loading" the worn section through surgical interventions. Finally joint replacement is an option to remove the worn section of the knee and replace it with a smooth metal and plastic articulation, this may be part or all of the knee.
OA has a genetic component and this cannot be changed, but there are ways to decrease the other risk factors for arthritis.
These include keeping a healthy weight. Consider walking up or down stairs, the forces going across the knee cartilage is far greater than your body weight, and any additional kilograms equates to many additional kilograms of force across the cartilage. So keep active, walking and swimming are good for movement and weight control.
Injuries to other structures inside the knee, such as meniscal or ligament damage may cause certain areas of cartilage to take more load/force thus accelerating the wear in these areas. If you have had an injury like this feel free to talk to you primary care physician or Dr Drynan regarding you knee injuries.
When considering partial or total knee arthroplasty (replacement) the patient should understand a few important issues. The patients age and function and functional goals will be discussed along with the cartilage damage, location and options including non operative and operative with Dr Drynan. Together, you and Dr Drynan will discuss function after the treatment, rehabilitation, long term outcomes and revision rates. You, the patient will make an informed decision regarding the best option for you, and your knee.
A total knee arthroplasty is replacing the distal femur and proximal tibia with metal implants, with a smooth highly crosslinked polyethylene plastic in the middle.
A partial knee replacement includes, the patella femoral joint, or part of the femoro-tibial joint (knee joint). Dr Drynan will discuss with you the options for treatment, risks, outcomes and likely course of recovery.
Adults and Paediatric populations may have areas of cartilage damage or loss of function. Occasionally this is due to trauma or injury. These situations may lead to loose bodies, joint effusions (swelling) and occasional locking of the knee. Larger cartilage defects may benefit from repair or reconstruction (replacement with cartilage from else where on the body or donated cartilage.
Osteochondritis Dissecans is a condition of the supportive bone under the cartilage of the knee, and elbow, commonly. This lack of supportive bone sometimes allows the cartilage to not be supported appropriately and may lead to loose bodies, cartilage defects, effusions, pain and degeneration.
Dr David Drynan Orthopaedic Surgeon
Sydney