Signed in as:
filler@godaddy.com
Signed in as:
filler@godaddy.com
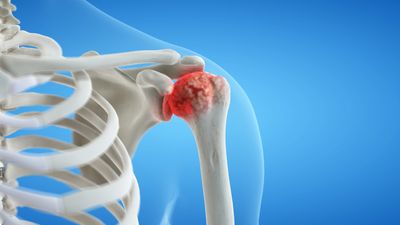
Arthritis means inflammation of the joint. Osteoarthritis is joint derangement due to cartilage loss. The loss of cartilage maybe due to age related degeneration, rotator cuff disease, trauma, infection, loss of bone support for cartilage and commonly instability. This leads to a loss of the smooth, pain-free gliding associated with a normal joint, resulting in a swollen, inflamed, stiff, painful joint with limited motion. This is in part due to direct mechanical pressure on the subchondral bone and oedema and in part due to the inflammatory process of cartilage degeneration. Some upper extremity pain is associated with the limited function of one joint compensated with other joints.
The natural history of Osteoarthritis is one of slow progression. Currently, although many scientist and doctors are working on this, there is no way to reverse cartilage loss reliably. Cartilage substitution from other areas is useful in bone defects following dislocations and fractures, or stimulation of fibrocartilage is possible.
The normal clinical progression of Osteoarthritis is of increasing pain and stiffness and limited function. Gradually as the movement become more restricted, the pain may ease slightly due to the severe limitation in movement, thus the function would be minimal.
Often the diagnosis is made clinically, with your doctor taking a history and performing an examination. This often confirmed with X-Rays, occasionally with CT or MRI scans. These latter scans often are looking to rule in or out other conditions that sometimes go with arthritis, such as rotator cuff tears and glenoid wear patterns
The goal of management of most shoulder conditions is to restore movement, improve pain and function. With shoulder arthritis the management depends on the underlying cause of the arthritis often and how advanced the condition is.
Initial treatment:
Goal to maintain function and improve pain:
Advanced stetting:
Goal to restore movement, allow function and improve pain.
Anatomic total shoulder arthroplasty is the removal of the arthritic humeral head and worn sections of the glenoid and replacing them with metal on the humeral side and plastic on the glenoid side. This done via an open incision over the front of the shoulder. The rotator cuff is essential in maintaining a balanced anatomic total shoulder arthroplasty, and as such it will be checked pre operatively and the rehabilitation will focus on rotator cuff function and shoulder range of motion.
Longevity of any arthroplasty has many factors, but the 2020 AOA National Joint Registry Data for the survival of 87.8% at 10 years for total shoulder stemmed prostheses. Talk to Dr Drynan about interpreting these results and your specific situation.
Reverse total shoulder arthroplasty entails removal of the arthritic humeral head and glenoid and replacing the original concave glenoid with a sphere (glenosphere) and the humeral head with a cup that allows the shoulder to function with the use of the deltoid and mechanics. This revolutionary design from started with Neer in 1970's and was re-envisioned with Grammont in 1985 improving function and survival of the implants dramatically. Multiple methods and iterations fo the designs of arthroplasty exist now to include computer modelling and planning with guidance and virtual reality possible with implanting the replacement.
Dr David Drynan Orthopaedic Surgeon
Sydney